- Dietary choices significantly impact arthritis symptoms, with certain foods and drinks known to exacerbate inflammation and pain.
- Key items to avoid include added sugars, processed meats, ultra-processed foods and sugar-sweetened beverages.
- An anti-inflammatory diet, similar to the Mediterranean or DASH diet, rich in plants, fish and whole grains, can help manage the condition.
- Lifestyle factors like weight management, physical activity and stress reduction are also crucial components of arthritis care.
- Individuals should consider dietary changes gradually and in consultation with a healthcare provider to find the most effective personal strategy.
The inflammatory culprits: Foods that can worsen symptoms
Extensive research and clinical observation have identified a consistent group of dietary offenders that may worsen arthritis symptoms. Highly processed foods are a primary concern, as they are often rich in refined grains, added sugars and unhealthy fats—all linked to increased systemic inflammation and obesity, a known risk factor for arthritis progression. Similarly, processed meats have been associated with elevated markers of inflammation in the body. Beyond solid foods, beverages play a significant role; sugar-sweetened drinks and excessive alcohol consumption can increase inflammation and, in the case of gout, raise uric acid levels. The common thread is their contribution to an inflammatory internal environment that can aggravate joint discomfort.The science of synovial sabotage
The mechanism by which diet influences joints is rooted in biochemistry. Certain foods can promote the production of pro-inflammatory cytokines—signaling proteins that drive the inflammatory response. For instance, diets with an imbalanced ratio of omega-6 to omega-3 fatty acids, common with high consumption of certain vegetable oils, can tip the body toward a state of chronic, low-grade inflammation. Furthermore, compounds like advanced glycation end products (AGEs), formed when foods are fried, grilled, or roasted at high temperatures, can accumulate in the body and induce oxidative stress, damaging tissues including those in the joints. This scientific understanding moves dietary advice beyond anecdote into evidence-based intervention.Building an anti-arthritis plate: Principles of an anti-inflammatory diet
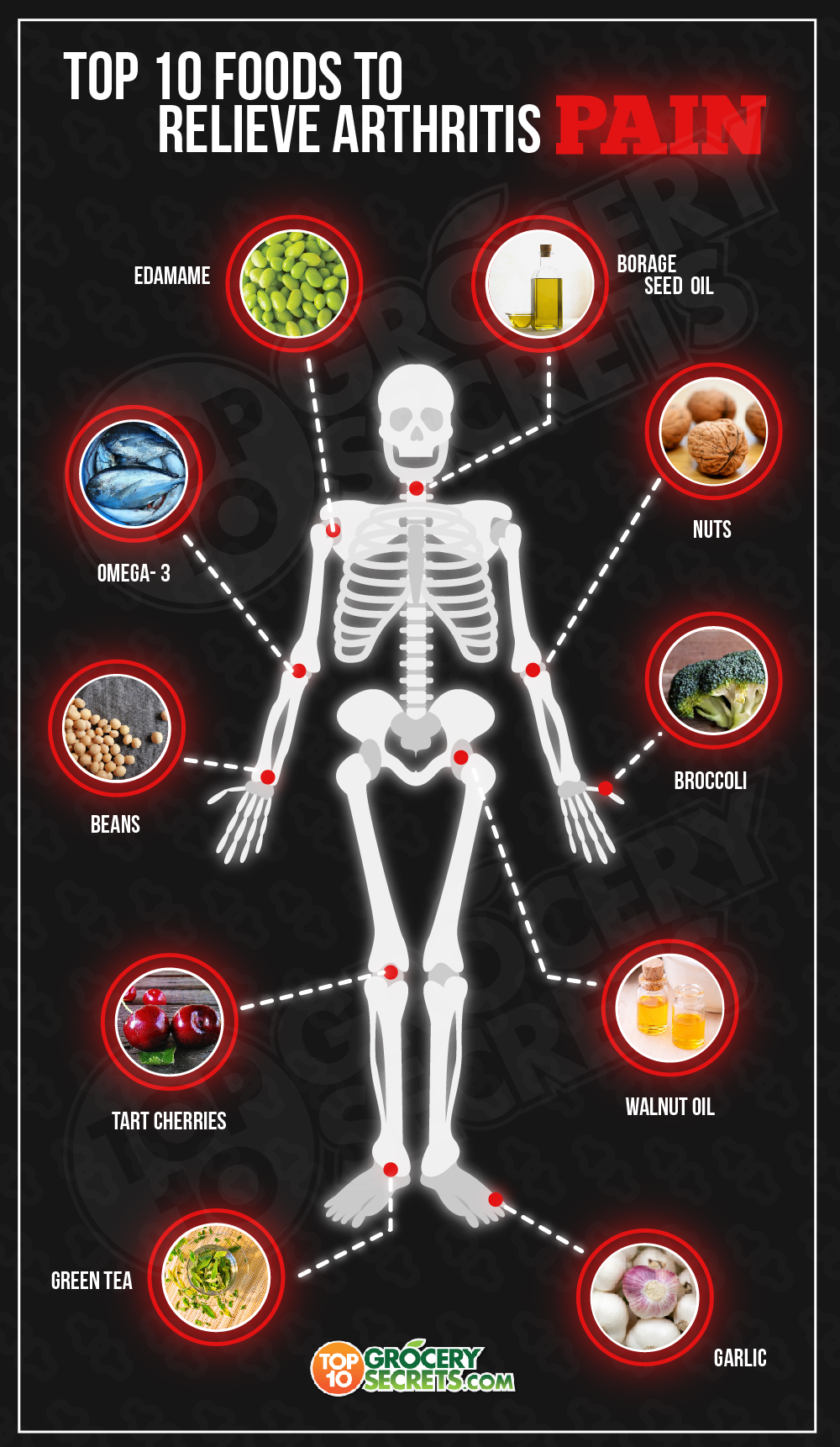
In contrast to the modern processed diet, an anti-inflammatory dietary pattern focuses on whole, nutrient-dense foods. This approach closely mirrors the celebrated Mediterranean Diet, which emphasizes fruits, vegetables, legumes, whole grains, nuts, seeds and fatty fish like salmon and mackerel rich in omega-3s. These foods provide a symphony of anti-inflammatory compounds: antioxidants that combat cellular damage, fiber that supports a healthy gut microbiome, and polyphenols that modulate inflammatory pathways. The goal is not to seek a single "superfood," but to adopt a consistent pattern of eating that collectively dampens inflammation and supports joint health.Navigating change: A gradual and sustainable approach
Adopting a new way of eating requires a strategic and patient approach. Health experts caution against abrupt, radical dietary overhauls, which can be unsustainable and may even trigger temporary detoxification symptoms like headaches or increased stiffness. A more effective method involves gradual substitution: slowly replacing ultra-processed snacks with whole-food alternatives, introducing more plant-based meals each week, and experimenting with herbs and spices for flavor instead of relying on salty or sugary sauces. This gradual shift allows the palate and digestive system to adapt, fostering long-term adherence.A holistic vision for joint health
Ultimately, managing arthritis through diet is one piece of a larger puzzle. Nutritional strategies work best when integrated with other vital lifestyle factors, including maintaining a healthy weight to reduce mechanical stress on joints, engaging in regular low-impact physical activity to preserve mobility, and managing stress and prioritizing sleep, both of which influence inflammatory pathways. This comprehensive view acknowledges that while food is a powerful tool, it operates within the broader context of daily life. For individuals navigating the challenges of arthritis, this evolving understanding offers a proactive and empowering path forward, turning everyday meals into an opportunity for relief and improved quality of life. Sources for this article include: Healthline.com PubMed.com MassGeneralBrigham.orgRoutines that Emphasize Natural, Non-Pharmaceutical Approaches Support Skin Health
By Petra Stone // Share
Study Examines Brain-Derived Protein Release Following 30-Minute Exercise Session
By Petra Stone // Share
Radish: An ancient, nutrient-packed root vegetable that belongs in modern kitchens
By Evangelyn Rodriguez // Share
Gaza's "Board of Peace" holds zero dollars despite billions pledged
By avagrace // Share
US to Reduce Military Commitments to NATO, Officials Say
By garrisonvance // Share
Colombian mercenaries trained at UAE bases fueling Sudan's genocide, new report reveals
By jacobthomas // Share
The Great Taking: A review of the coming collapse we all refuse to see
By bellecarter // Share
Breakthrough: Abundant Element Outshines Rare Metals in Advanced Chemical Synthesis
By morganverity // Share
Study: 560-610 Minutes of Weekly Exercise May Cut Cardiovascular Risk by Over 30%
By petrastone // Share