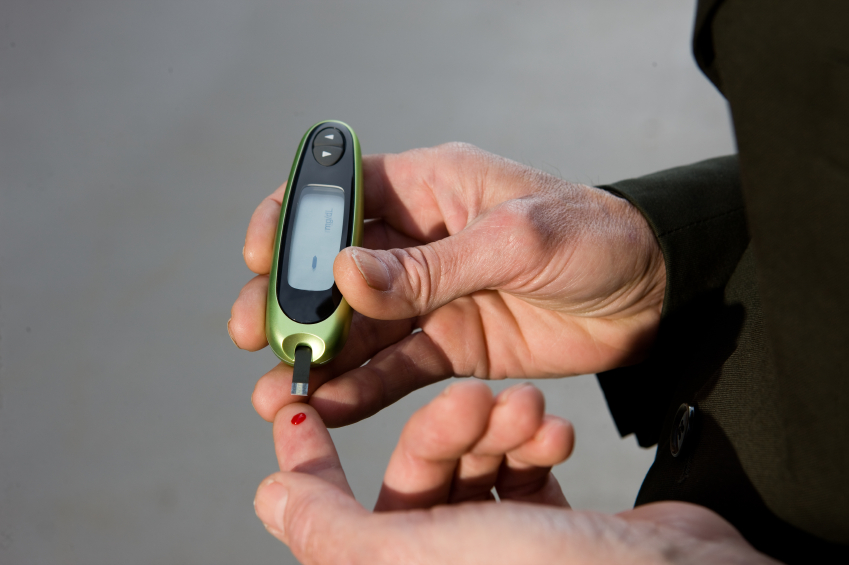
- Less than 7% of U.S. adults have optimal cardiometabolic health.
- High consumption of ultraprocessed foods is linked to a higher risk of Type 2 diabetes.
- The ability to switch between burning carbs and fats is essential for metabolic health.
- There are significant health disparities based on race, ethnicity and education.
- Early lifestyle changes can significantly reduce the risk of metabolic diseases.
The modern lifestyle’s perfect storm
Urban Kiernan, a doctorate holder in bioanalytical chemistry, highlights the challenges in defining "normal" metabolic health in an era where the baseline is skewed by widespread metabolic dysfunction. "When the vast majority are unwell, it’s hard to establish a true baseline," he says. The modern lifestyle, characterized by ultra-processed foods, sedentary habits, chronic stress and poor sleep, creates a perfect storm for metabolic imbalance. Karen Hawkins, a registered dietitian and certified diabetes educator, adds, "It’s very challenging to be physically active because of our lifestyle. We drive everywhere and do very little walking."Defining metabolic health
Metabolic health is not just about weight. Dr. Saremi explains, "You don’t need to look metabolically unhealthy to be metabolically unhealthy." Key biomarkers used to assess metabolic health include fasting blood sugar, blood pressure, lipid profile and waist circumference. Lean muscle mass, often overlooked, is also crucial. A metabolically healthy person can manage their weight, maintain steady blood sugar levels and efficiently use energy. Metabolic flexibility—the body's ability to switch between burning carbohydrates and fats—is a vital component. This flexibility ensures that the body can handle a carb-heavy meal without a prolonged blood sugar spike and efficiently tap into stored fat when needed.The impact of ultra-processed foods
A population-based study published in JAMA Internal Medicine found a 5% increase in Type 2 diabetes risk for every extra 100 grams of ultra-processed food consumed daily. Hawkins emphasizes the importance of whole, unprocessed foods: "If you are eating carbs, it’s important to do so in a responsible way. Complex and fiber-rich carbs like vegetables and fruits digest slowly, helping steady blood sugar levels."Building metabolic balance
Achieving metabolic health requires intentional choices in diet, exercise and lifestyle. Dr. Saremi advises, "Build your meals around whole, unprocessed foods. Timing your carbs is important, too. Eating higher-carb meals around workouts can improve glucose handling." Hawkins recommends meal prepping to make healthy eating sustainable: "It doesn’t have to be complicated. Steam some salmon, roast vegetables, build a salad—anything you can portion out for the week helps." Regular physical activity is non-negotiable. Dr. Saremi highlights the importance of non-exercise activity thermogenesis (NEAT), which includes everyday movements like walking and climbing stairs. "Small changes, like parking farther away or taking the stairs, add up," he says.Addressing health disparities
The study by Tufts University also revealed significant health disparities. Adults with less education were half as likely to have optimal cardiometabolic health compared to those with more education. Mexican Americans had one-third the optimal levels compared to non-Hispanic white adults. Dr. Dariush Mozaffarian, dean of the Friedman School, stresses the need to address these disparities: "Social determinants of health such as food and nutrition security, social and community context, economic stability and structural racism put individuals at an increased risk of health issues."A call to action
Metabolic health is not a fixed state but a spectrum. With the right tools, individuals can move in a positive direction. Dr. Saremi concludes, "Health is a lot more than specific numbers or metrics. You have to look at the whole picture—your lifestyle, work, activity level, diet, relationships, community and how much sleep you’re getting." Lifestyle and culinary medicine, as Hawkins suggests, are key to managing metabolic health and preventing chronic diseases. Early intervention and consistent, sustainable changes can significantly improve health outcomes and well-being. The crisis of metabolic dysfunction requires urgent action, but the potential for positive change is within reach. Sources for this article include: TheEpochTimes.com Tufts.edu JAMAnetwork.com PubMed.govNavigating the world of nutritional supplements: A guide to informed choices
By Kevin Hughes // Share
Unveiling lecithin: The versatile emulsifier bridging nutrition and food science
By Laura Harris // Share
What are the benefits of moringa oleifera?
By News Editors // Share
In the dark: How even dim nighttime light rewires your health — from cancer to diabetes
By Willow Tohi // Share
Possible deadly virus exposure at NIH lab raises new biosecurity concerns
By isabelle // Share
Where did the term “ultra-processed food” come from?
By ljdevon // Share
The Silver Singularity: A review of the book that sees through the matrix
By bellecarter // Share
Putin Concludes Beijing Visit With 42 Bilateral Agreements, Stronger Russia-China Ties
By garrisonvance // Share